Cyclocryotherapy
OverView
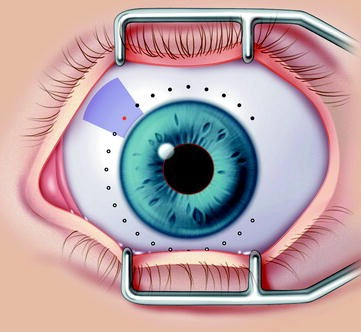
Cyclocryotherapy, also known as cyclocryoablation, is a procedure used to treat certain types of glaucoma by reducing the production of aqueous humor, the fluid inside the eye that maintains intraocular pressure (IOP). This treatment involves applying extreme cold to the ciliary body, a part of the eye responsible for producing aqueous humor, to destroy or impair some of the tissue, thereby lowering the IOP.
Understanding Glaucoma and the Role of Cyclocryotherapy
What is Glaucoma?
- Glaucoma is a group of eye conditions that damage the optic nerve, often due to elevated IOP. Over time, this damage can lead to vision loss and blindness if not effectively managed.
Indications for Cyclocryotherapy:
- Cyclocryotherapy is typically reserved for cases of glaucoma that have not responded well to other treatments, such as medications, laser therapies, or conventional surgeries. It is often used in advanced or refractory glaucoma, where conventional methods have failed to control the IOP.
The Cyclocryotherapy Procedure
Cyclocryotherapy is usually performed as an outpatient procedure, often under local anesthesia with sedation.
Preparation:
Pre-Operative Assessment:
- The ophthalmologist will conduct a thorough examination of the eye, including measuring the IOP and assessing the overall health of the eye.
Anesthesia:
- Local anesthetic is administered to numb the eye and surrounding tissues. Sedation may also be given to help the patient relax during the procedure.
The Procedure:
Cryoprobe Application:
- A cryoprobe, a device that delivers extreme cold (often using liquid nitrogen or nitrous oxide), is applied to the sclera (the white part of the eye) overlying the ciliary body. The freezing temperature is transmitted to the ciliary body, causing localized destruction of the tissue responsible for producing aqueous humor.
Treatment Area:
- The cryoprobe is typically applied to several spots around the eye, covering a portion of the ciliary body, usually around 180 to 270 degrees of the eye's circumference, depending on the severity of the condition.
Duration:
- The freezing cycle lasts for several seconds at each application site, and the entire procedure typically takes 15-30 minutes.
Post-Procedure Care:
Eye Patching:
- The eye may be patched after the procedure to protect it and promote healing.
Medications:
- Post-operative care usually includes the use of anti inflammatory and antibiotic eye drops to reduce inflammation and prevent infection.
Pain Management:
- Some patients may experience discomfort or pain after the procedure, which can be managed with prescribed pain relievers.
Benefits of Cyclocryotherapy
Reduction of Intraocular Pressure:
- The primary benefit of cyclocryotherapy is its ability to lower IOP in cases of severe or refractory glaucoma, helping to prevent further damage to the optic nerve and preserve vision.
Alternative for Severe Cases:
- Cyclocryotherapy offers an option for patients who have not responded to other treatments, providing an alternative when conventional surgeries or medications are ineffective.
Non-Invasive:
- Compared to more invasive surgical options, cyclocryotherapy is relatively less invasive, as it does not require incisions inside the eye.
Risks and Potential Complications
While cyclocryotherapy can be effective, it also carries certain risks and potential complications:
Inflammation and Pain:
- Post-procedure inflammation and pain are common and usually managed with medication, but severe pain or prolonged inflammation may occur in some cases.
Hypotony:
- Excessive lowering of IOP, known as hypotony, can occur if too much ciliary body tissue is destroyed. This can lead to a soft eye, which may cause visual disturbances and other complications.
Phthisis Bulbi:
- In rare cases, severe damage to the ciliary body can lead to phthisis bulbi, a condition where the eye becomes shrunken and non-functional.
Loss of Vision:
- Although cyclocryotherapy is intended to preserve vision by lowering IOP, there is a risk of vision loss due to complications from the procedure itself.
Inflammation in Adjacent Tissues:
- The extreme cold used in the procedure can inadvertently affect surrounding tissues, leading to unintended damage.
Rebound Glaucoma:
- In some cases, the IOP may rise again after initially responding to the treatment, necessitating further intervention.
Post-Procedure Expectations and Follow-Up
Monitoring:
- Regular follow-up visits are essential to monitor IOP and assess the effectiveness of the procedure. Additional treatments may be required if the IOP is not adequately controlled.
Vision Changes:
- Patients may experience some changes in vision after the procedure, including blurring or decreased vision, which should be discussed with the ophthalmologist.
Activity Restrictions:
- Patients may be advised to avoid strenuous activities and protect the eye from injury during the healing process.
Conclusion
Cyclocryotherapy is a valuable treatment option for managing severe or refractory glaucoma cases where other treatments have failed. By selectively destroying the ciliary body tissue responsible for producing aqueous humor, this procedure can significantly reduce IOP and help preserve vision in patients with advanced glaucoma. However, due to the potential risks and complications, it is typically reserved for cases where the benefits outweigh the risks. Patients should have a thorough discussion with their ophthalmologist to understand the procedure, its potential outcomes, and the necessary post-operative care.
USEFUL LINKS
SANKALP HOSPITALS PVT. LTD.
Vijay Smruti, Town Hall Circle, Jamnagar - 361 001 (Gujarat) INDIA
sankalphospitals@gmail.com
0288 2553435
© 2024 Sankalp Hospitals Pvt. Ltd.
